BenePath® Enrollment Platform

Seamless, one-stop eligibility and enrollment
Health and Human Services (HHS) agencies must keep ahead of evolving social service demands. They need modern, consumer-driven solutions, along with expert guidance and support to overcome their most daunting service delivery challenges.
Our BenePath Enrollment Platform can help clients transform the delivery of services with a seamless, one-stop eligibility and enrollment platform designed to integrate back-office CRM with front-office contact center operations. By leveraging artificial intelligence (AI) and robotic process automation (RPA), government agencies can better serve constituents with reduced turnaround times, expedited access to benefits and enhanced federal, state and local regulatory compliance.
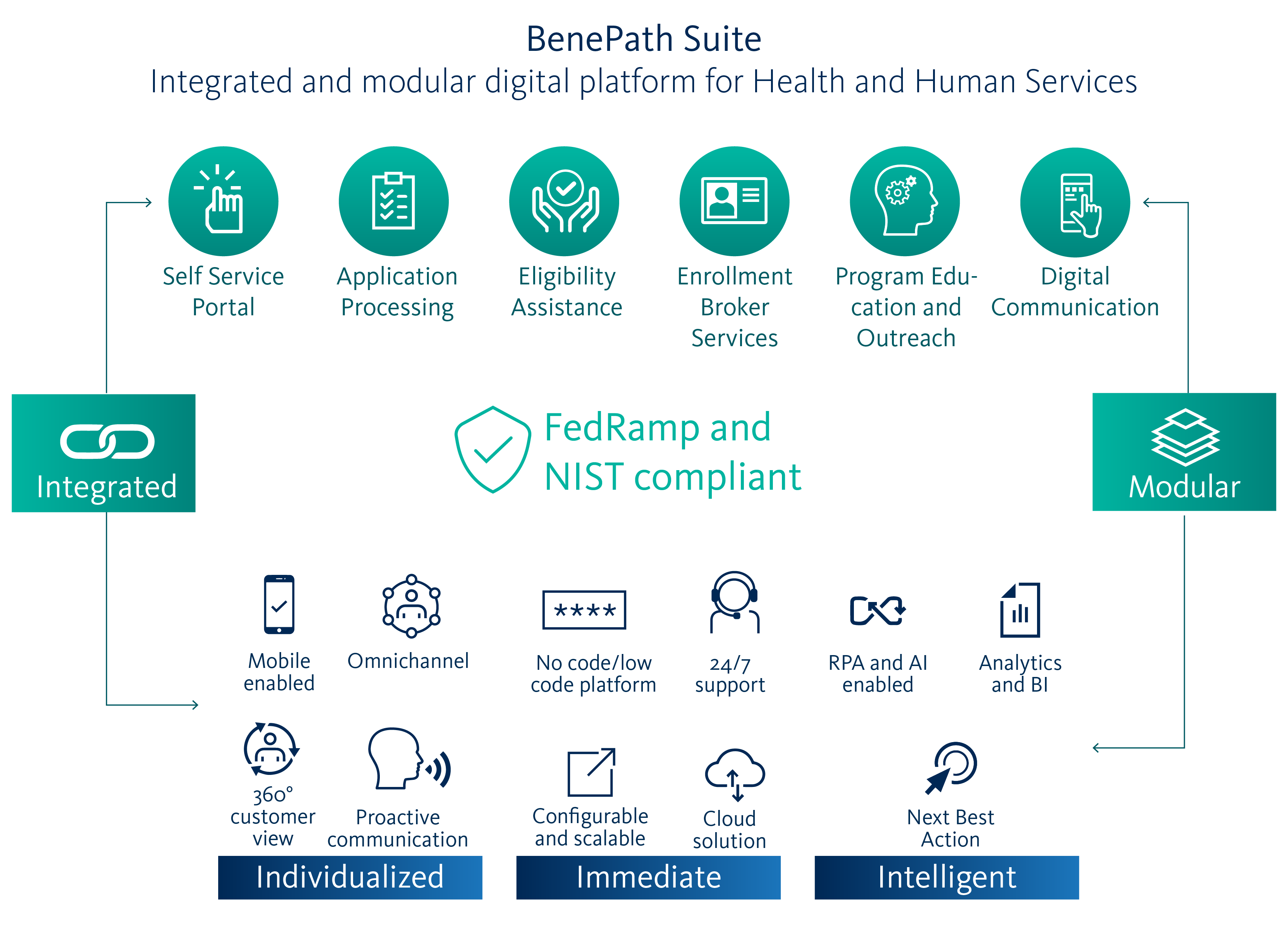
Integrated and modular digital platform for health and human services
Traditionally siloed social services and fragmented, manual processes that are not human-centered inevitably fail to deliver timely services to those in need. Government agencies recognize the need to make every constituent interaction better. Our BenePath suite offers a comprehensive, integrated customer service solution that consists of two products, our Self-Service Portal and Eligibility and Enrollment Platform. Using our suite, agencies gain seamless, one-stop eligibility and enrollment capable of integrating across all available platforms. Because our suite is modular and configurable, we can partner with agencies to help streamline your state’s health and human services ecosystem, modernizing service delivery, adding momentum to your mission, and improving program outcomes.
